

The infrastructure for chronic care management is largely in place. Health systems have invested in remote monitoring programs, care management teams, and risk stratification tools.
What hasn't worked is the architecture: data intelligence and care delivery were built as separate systems, and when they don't operate as one, the loop never closes. Insight stops short of action, action stops short of outcomes, and policy is demanding proof of the entire chain.
Most platforms today fall into two categories: analytics-driven or care management. One delivers data without execution. The other delivers human outreach without intelligent prioritization.
Chronic care requires both working as one system: from data to action to measurable outcomes.
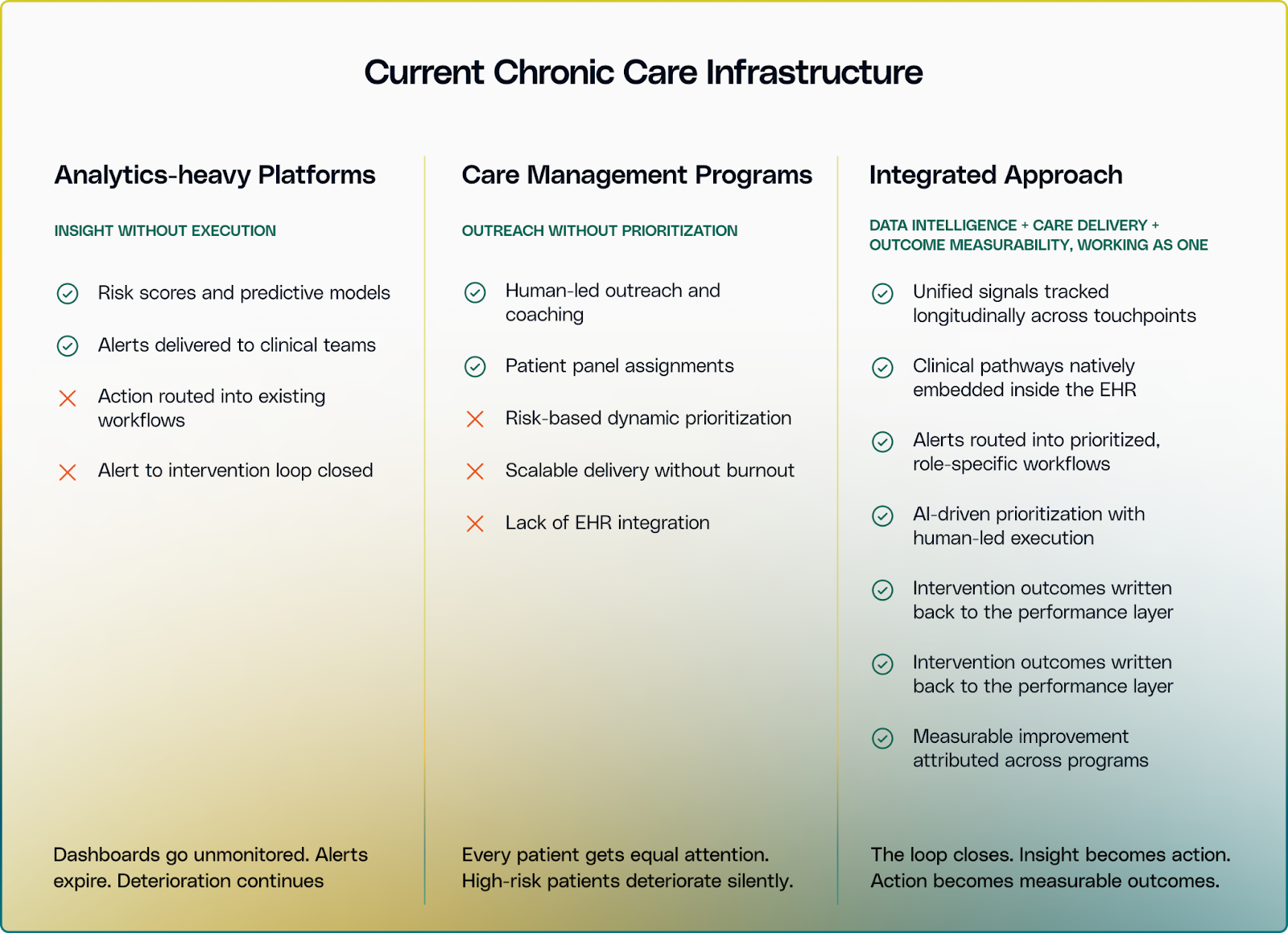
Story Health by Innovaccer operationalizes continuous care by embedding intelligence and delivery into the clinical workflows your teams already use.
When home readings live outside the EHR, clinicians reconcile timelines and decide what matters under time pressure. That is how drift becomes a delay.
Story Health eliminates that gap by unifying RPM device readings, medication history, labs, and patient symptoms into one EHR-native view. Data, documentation, and care plan updates organize into a single longitudinal timeline. Visibility is the first move. The real shift happens when signals route into prioritized action.
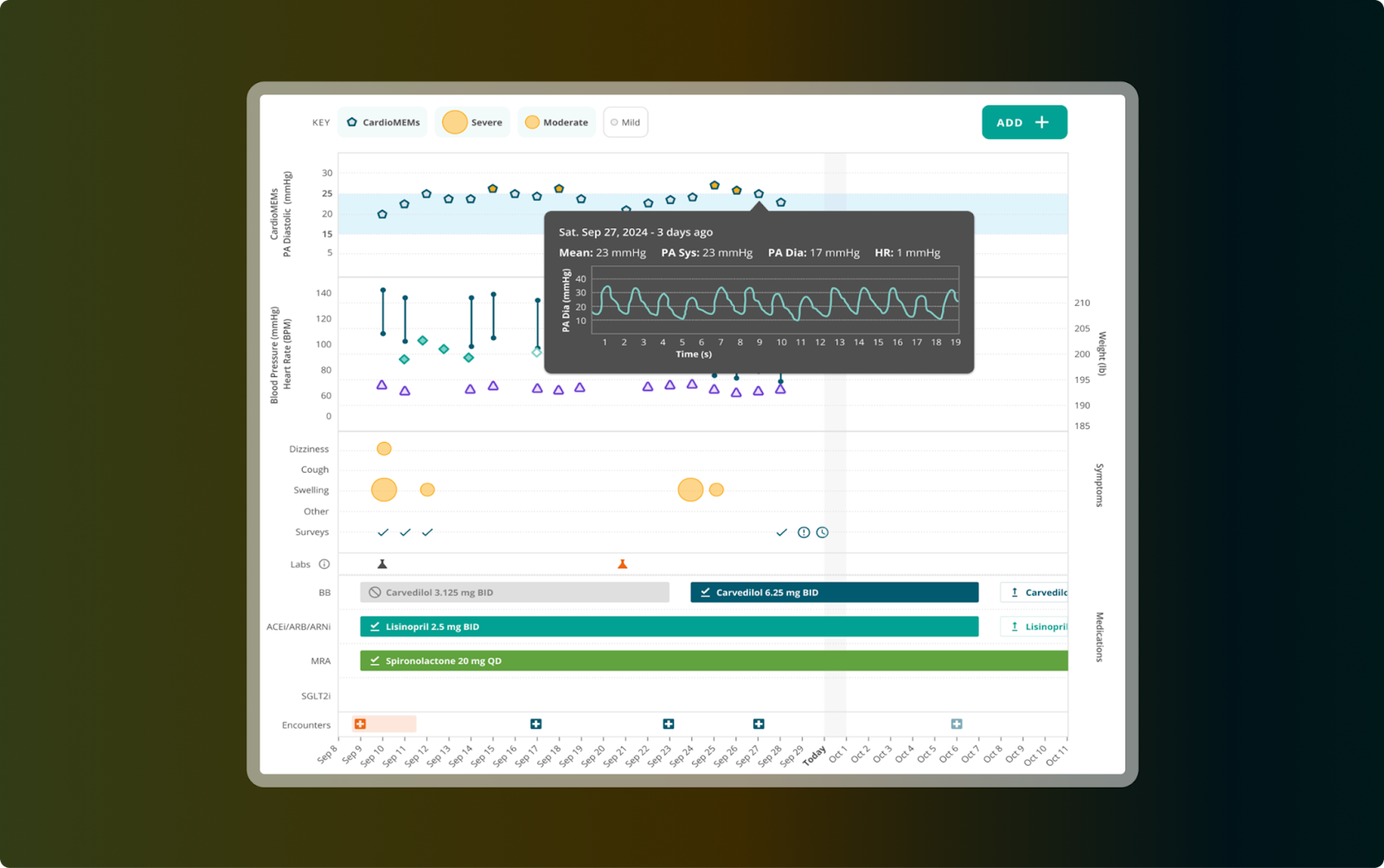
Story Health monitors the unified timeline continuously. When home readings show meaningful drift, AI analyzes medication history, lab trends, symptom patterns, and recent clinical events to surface who needs attention and why; triaged by severity, trajectory, and clinical context.
The prioritized decision routes into the EHR with a recommendation: adjust dosage, modify titration, escalate for specialist review. Your provider reviews the patient's complete history and chooses to accept, modify, or reject it. Clinical authority stays intact. What changes is that clinicians spend time on decisions, not data hunting.
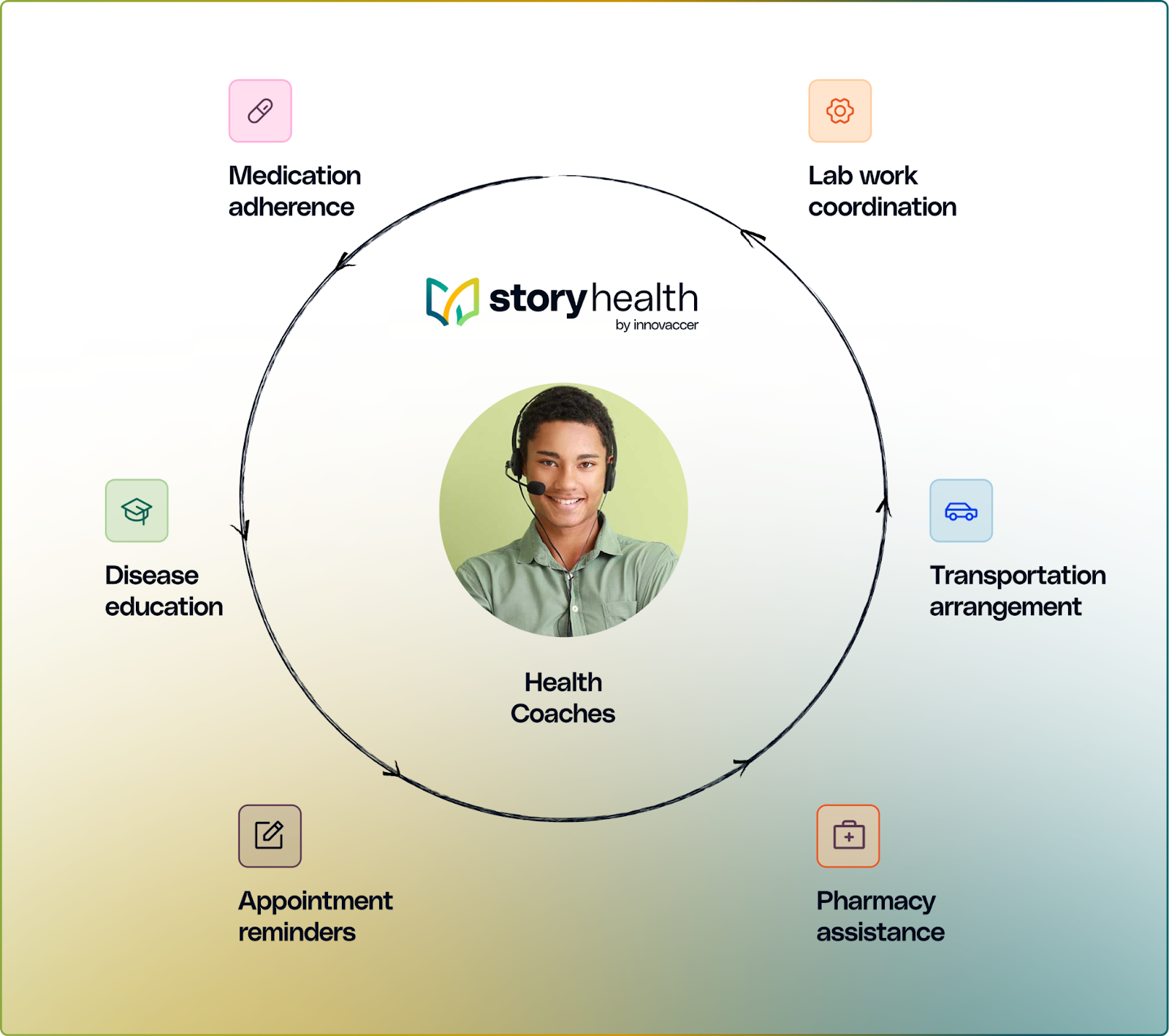
Most RPM programs stop at data collection and leave execution to manual workflows. Story Health closes the loop by embedding virtual care teams that own follow-through between visits.
When a provider accepts a medication adjustment, Story Health sends an automated alert to the patient. Then the health coach manages adherence, symptoms, and provides support to the patient to drive outcomes. Coaches handle routine friction such as medication adherence, lab coordination, appointment reminders, patient questions, and escalate what requires clinical judgment. Routine follow-through scales without adding clinical FTEs.
The system recommends and prioritizes. Clinicians decide. You maintain the governance model required to run continuous care safely at scale.
Atlas integrates EHR, claims, labs, pharmacy, and device data into a single longitudinal patient record. It handles attribution, risk stratification, baseline setting, and outcome tracking across conditions, care settings, and payment models.
Together, Atlas and Story Health create closed-loop infrastructure: Atlas unifies data and prioritizes risk, Story Health delivers coordinated care, and both systems track measurable outcomes longitudinally. You align the data foundation with the care delivery layer from the start, rather than layering continuous care programs onto fragmented infrastructure.
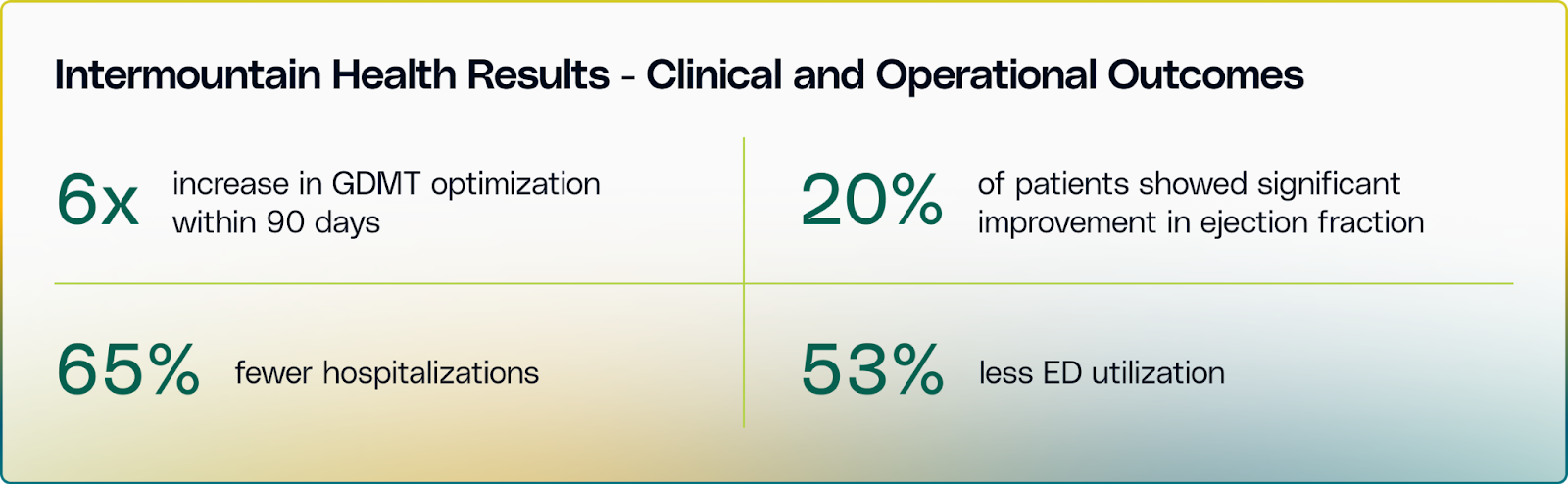
Intermountain Health had a nationally recognized heart failure disease management (HFDM) program. The remaining gap was GDMT optimization at scale: getting more patients to medication targets faster, without adding clinic visits that their appointment capacity could not absorb.
Read the full case study here →
This is the value proposition executives care about: fewer avoidable events, protected specialist capacity, and measurable improvement that holds over time.
Chronic disease will keep forcing margin pressure and capacity constraints. You can respond with fragmented tools and manual processes, or you can build continuous care infrastructure designed for longitudinal performance.
Story Health and Atlas provide infrastructure that measures trajectory, coordinates action, and proves improvement across the payment models you already manage today. The health systems that close the gap between chronic care investment and measurable outcomes will not do it by adding more tools. They will do it by aligning the data layer with the execution layer from the start.
See how Story Health and Atlas work in your environment. Schedule a personalized demo.